Frequently asked questions about cerebral embolic protection & the SENTINEL™ Cerebral Protection System
What does the SENTINEL Cerebral Protection System (CPS) do?
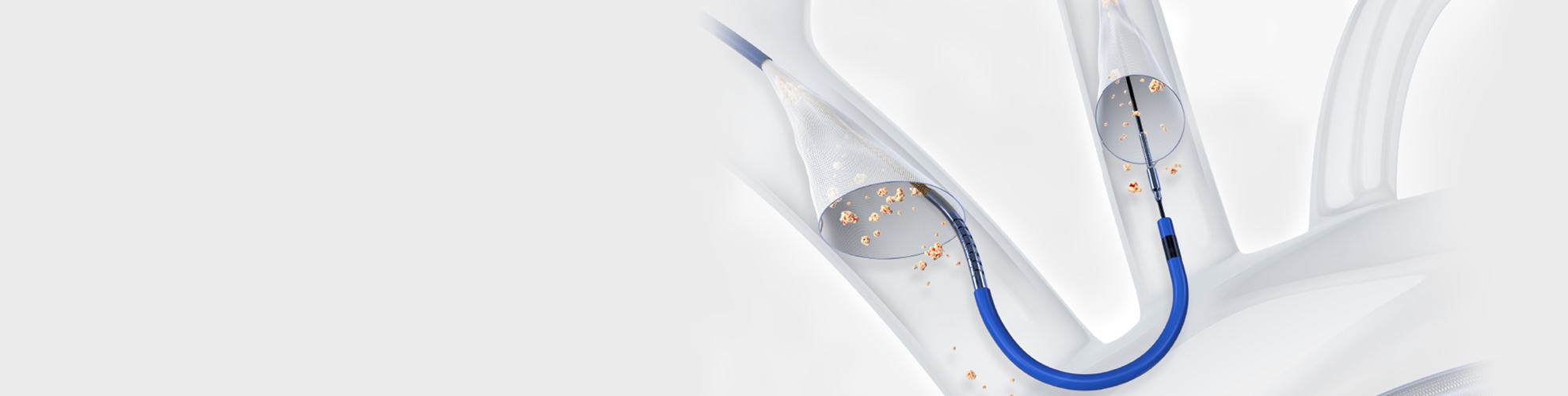
SENTINEL CPS works by capturing and removing embolic debris dislodged during the TAVR procedure, before it can reach the brain.
How can I find a center that offers Protected TAVR™ with the SENTINEL™ Cerebral Protection System?
Not every hospital that performs TAVR offers cerebral embolic protection. Find a medical center near you using the center finder tool.
What happens to the debris if it is not collected?
When the debris from the TAVR procedure is not collected, it can travel in the bloodstream toward the brain. If the debris material reaches the brain, stroke may occur.
What is the benefit of cerebral embolic protection?
Patients who undergo TAVR with the SENTINEL CPS have a significantly higher rate of stroke-free survival than do patients who undergo TAVR without the device. In fact, SENTINEL CPS captured visible embolic debris headed toward the brain in 99% of TAVR cases.1
What is left behind in cerebral embolic protection?
Nothing. Once the replacement valve is in place the SENTINEL device, along with all the debris it collected, are completely removed from the body.
Is cerebral embolic protection safe?
Yes. Clinical trials involving more than 3,500 patients have demonstrated that the SENTINEL device is safe and effective. The SENTINEL cerebral protection technology has been used to protect thousands of patients worldwide and is the most-studied embolic protection device in its field.
Is the SENTINEL device FDA approved?
Yes, it was approved on June 5, 2017.
Does cerebral embolic protection add to my recovery time?
No, having cerebral embolic protection will not impact your recovery time.
Does insurance cover TAVR and Protected TAVR with Sentinel?
Most insurers cover the diagnosis and medically necessary treatment of aortic valve disease. Medicare has a national policy for severe aortic valve stenosis, which includes coverage for TAVR and Protected TAVR. Private insurance coverage for TAVR procedures varies so work with your doctor’s office and insurance carrier to check coverage levels prior to receiving treatment.
Navigating insurance payments can be tricky and confusing. It is best to check with your provider and insurance carrier before you undergo the procedure to understand what your insurance will cover and what costs you may incur.
How can I find out if my insurance company will cover the use of SENTINEL with my TAVR procedure?
Boston Scientific recommends that you work with your physician’s office to verify insurance coverage and benefits prior to the TAVR procedure being performed.
If you are covered by Medicare & Medicaid, The Centers for Medicare & Medicaid Services (CMS) covers transcatheter aortic valve replacement (TAVR) under a national policy. However, certain conditions must be met. Please speak with your heart team to ensure that you and the facility where you have your procedure meet the conditions outlined by CMS.
If you have a Medicare Supplement Plan, we recommend verifying with your plan in advance of the scheduled procedure. Medicare Supplement insurance plans are designed to work with Medicare and can assist in out-of-pocket costs that Original Medicare (Part A and Part B) does not pay, such as: coinsurance, copayments, and deductibles.
If you have private insurance or Medicare Advantage plans, we recommend a verification of benefits be done with your insurance company several days, if not weeks, in advance of the scheduled procedure. The verification of benefits is a crucial component to understanding the exact coverage criteria under your plan. Your plan may require additional information or authorizations. These processes are meant to allow your health insurance company the opportunity to evaluate your treatment plan and specifics of the request to review for medical necessity. Please ask your care provider about your anticipated coverage options.
Is there financial assistance available for the TAVR procedure with SENTINEL for Protected TAVR
Since there is widespread insurance coverage for TAVR procedures, there is no formal patient financial assistance program available for the TAVR and Protected TAVR with SENTINEL procedure at this time.
What are the different kinds of stroke?
A transient ischemic attack (TIA) is often called a mini stroke. It’s a brief interruption of blood flow to part of the brain, spinal cord or retina, which may cause temporary stroke-like symptoms but does not damage brain cells or cause permanent disability. Symptoms of TIA usually last only a few minutes but may persist for up to 24 hours. The risk of stroke is especially high within 48 hours after a TIA.
An ischemic stroke is the most common type of stroke. It happens when blood flow through the artery that supplies oxygen-rich blood to the brain becomes blocked. Blood clots often cause the blockages that lead to ischemic strokes. The effects of a stroke vary, and can depend on which part of the brain was injured and how long it took to get medical attention.
The most common effects from stroke include cognitive difficulties, paralysis, weakness, as well as difficulty with language, vision, and swallowing.
As with any medical device, there are risks associated with use of the SENTINEL Cerebral Protection System. These risks include but are not limited to: infection, blood vessel injury, stroke, death.
Issues specific to the use of the SENTINEL have been reported in a small number of patients and typically went away in 30 days. The use of SENTINEL during yourprocedure is solely at the discretion of your doctor.
1 SENTINEL Clinical Trial